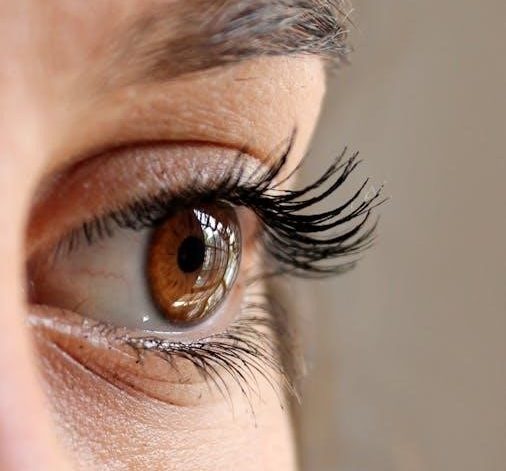
Suture Needle Size Guide: A Comprehensive Overview (Updated 03/31/2026)
Navigating suture selection is crucial for optimal wound healing. This guide details USP and metric systems‚ aiding clinicians in choosing appropriate sizes for varied surgical needs‚
especially microsurgical repairs.
Selecting the correct suture needle size is paramount in achieving successful wound closure and minimizing complications. This involves understanding the interplay between needle diameter‚ point type‚ and curvature‚ all tailored to the specific tissue being repaired.
Suture sizes directly impact tissue trauma‚ tensile strength‚ and cosmetic outcomes.
Clinicians must consider factors like tissue type‚ anatomical location‚ and patient characteristics – including age – to optimize suture choice.
Sizes range dramatically‚ from extremely fine needles (11-0) used in ophthalmology to larger sizes for robust tissues.
Understanding Suture Size Nomenclature (USP vs. Metric)
Suture sizes are quantified using two primary systems: the United States Pharmacopeia (USP) and the metric system. The USP system employs a numerical designation with “0” representing a larger size; thus‚ 6-0 is smaller than 2-0. Conversely‚ the metric system utilizes millimeters (mm) to directly indicate suture diameter.
Understanding both systems is vital‚ as surgeons may encounter either in practice. Conversion charts facilitate translation between USP and metric equivalents‚ ensuring accurate suture selection for diverse clinical scenarios and minimizing potential errors.

USP Suture Size System
The USP system is historically dominant in the United States‚ defining suture size inversely proportional to its diameter. Larger numbers (e.g.‚ 1‚ 2‚ 3) denote thicker sutures‚ while the addition of zeros (e.g.‚ 6-0‚ 7-0) signifies progressively finer diameters.
This system allows for precise selection based on tissue fragility and desired tensile strength. Sizes range from 8-0 (very fine‚ for ophthalmic use) up to 7‚ though larger sizes are less common in modern surgical practice. Accurate interpretation is key for optimal wound closure.

Detailed Breakdown of USP Sizes: 6-0 to 11-0
The finer USP sizes‚ 6-0 to 11-0‚ are primarily utilized in delicate procedures. 6-0 is common for facial closures‚ offering good cosmetic results. Progressing to 7-0‚ 8-0‚ 9-0‚ and 10-0‚ sutures become increasingly refined‚ suitable for ophthalmic surgeries and microsurgical repairs.
11-0 represents the finest commercially available suture‚ reserved for specialized microsurgical applications. Understanding these nuances ensures appropriate tissue approximation and minimizes scarring.
Common USP Sizes and Their Applications
Several USP sizes find frequent application across surgical specialties. 3-0 and 4-0 are workhorses for general skin closures‚ providing adequate strength and minimizing dead space. 5-0 is often preferred for subcutaneous closures‚ reducing tension on epidermal layers.
Larger sizes‚ like 2-0 and 1-0‚ are employed for fascia‚ muscle‚ and heavily stressed tissues. The selection hinges on tissue type‚ location‚ and desired cosmetic outcome‚ ensuring optimal wound healing.

Metric Suture Size System
The metric system offers a direct correlation to suture diameter‚ expressed in millimeters. Unlike the inverse USP system‚ larger metric numbers indicate thicker sutures. This system provides a more intuitive understanding of suture size‚ simplifying communication and reducing potential errors.
Common metric sizes range from 0.9 to 6.0‚ with 0.9 representing a very fine suture and 6.0 a robust‚ heavy-duty option. This standardized approach enhances precision in surgical procedures globally.
Correlation Between USP and Metric Sizes
Understanding the relationship between USP and metric sizing is vital for seamless transitions. Generally‚ a USP size of 6-0 corresponds to a metric size of approximately 0.7 metric diameter. As USP numbers increase (e.g.‚ 7-0‚ 8-0)‚ the metric diameter decreases (e.g.‚ 0;5‚ 0.4).
Conversely‚ larger USP sizes (like 2-0‚ 3-0) equate to larger metric diameters (0.9‚ 1.0). Clinicians should utilize conversion charts for precise equivalence‚ ensuring accurate suture selection during procedures.
Advantages of the Metric System
The metric system offers a more straightforward‚ decimal-based approach to suture sizing. Unlike the USP system’s inverse numbering‚ larger metric values directly indicate larger suture diameters‚ reducing potential confusion. This linear progression simplifies calculations and promotes consistent sizing across international settings.
Furthermore‚ metric measurements are universally recognized‚ fostering better communication and standardization within the global medical community‚ ultimately enhancing patient safety and surgical precision.
Needle Point Types
Selecting the correct needle point is paramount for efficient tissue penetration and minimal trauma. Three primary types exist: tapered‚ cutting‚ and spiked. Tapered points excel in delicate tissues‚ spreading rather than cutting through. Cutting points‚ featuring a triangular blade‚ are ideal for tougher tissues like skin and fascia.
Spiked needles‚ though less common now‚ offer quick penetration but cause more trauma. The choice depends entirely on the tissue’s density and desired wound closure characteristics.

Tapered Needles: Uses and Benefits

Tapered needles are designed for tissues that bleed easily or require minimal trauma during penetration. Their smooth‚ gradually narrowing design allows them to slide through tissues with minimal disruption‚ making them ideal for delicate procedures like vascular repairs and intestinal anastomoses.
They excel in soft tissues‚ reducing the risk of tearing and promoting better coaptation. This design minimizes tissue damage‚ leading to improved healing and reduced scarring.
Cutting Needles: Uses and Benefits
Cutting needles possess a triangular or blade-shaped cutting edge‚ designed to penetrate denser tissues with minimal force. They are particularly well-suited for skin closure‚ tough fascia‚ and tendons where a precise‚ clean puncture is essential.
The cutting edge creates a pathway‚ reducing the need for excessive pressure and minimizing tissue drag. This characteristic makes them efficient for tissues that are difficult to penetrate‚ offering reliable performance.
Spiked (Traumatic) Needles: Uses and Considerations
Spiked needles‚ also known as traumatic needles‚ feature a sharpened point that splits tissue fibers as they pass through. Historically used‚ they are now less common due to the tissue damage they cause. Their primary application remains in heavily scarred or fibrous tissues where other needle types struggle to penetrate.
However‚ the traumatic action creates a larger wound track‚ potentially increasing post-operative pain and prolonging healing. Careful consideration is vital before selecting these needles.
Needle Body Characteristics
Beyond point type‚ needle characteristics significantly impact surgical technique and tissue handling. Length is crucial; shorter needles offer precision in confined spaces‚ while longer ones access deeper structures. Common lengths range from 30mm to 60mm‚ selected based on wound depth and surgical approach.
Curvature‚ expressed as a fraction of a circle (e.g.‚ 1/2‚ 3/8‚ 5/8)‚ dictates needle maneuverability. A 3/8 circle is versatile‚ while a 1/2 circle offers a wider bite.
Needle Length Considerations
Selecting the correct needle length is paramount for efficient and effective suturing. Shorter needles‚ typically 30-40mm‚ excel in areas with limited access‚ like cosmetic procedures or delicate facial repairs‚ offering enhanced control and minimizing tissue trauma.
Conversely‚ longer needles – 50-60mm – are ideal for deeper tissues and larger wounds‚ providing sufficient reach without excessive manipulation. Consider the depth and location of the wound when choosing.
Needle Curvature (1/2 Circle‚ 3/8 Circle‚ etc.)
Needle curvature significantly impacts maneuverability and surgical technique. 1/2 circle needles offer a broader arc‚ facilitating deep suture placement and wider wound access‚ proving useful in abdominal closures.
3/8 circle needles provide tighter turns‚ ideal for superficial tissues and areas requiring precise control‚ like skin closure. Straight needles are reserved for specialized applications‚ demanding direct insertion.
The chosen curvature should complement the surgical site’s anatomy and depth.
Suture Material and Needle Size Combinations
Selecting the correct suture material alongside the appropriate needle size is paramount for successful wound approximation. Monofilament sutures‚ known for minimal tissue drag‚ often pair well with smaller needle diameters‚ reducing tissue trauma during passage.
Conversely‚ multifilament sutures‚ offering superior knot security‚ can accommodate slightly larger needles. Absorbable sutures benefit from precise needle control‚ while non-absorbable options prioritize strength and durability‚ influencing size choices.
Monofilament vs. Multifilament Suture & Size Selection
Monofilament sutures generally require a slightly larger needle size compared to multifilament sutures of equivalent tensile strength. This compensates for their lower knot security and reduced tissue purchase.
Multifilament sutures‚ with their braided structure‚ offer better handling and knot holding‚ allowing for smaller needle diameters. Consider tissue reactivity; monofilaments minimize inflammation.
For delicate tissues‚ prioritize a smaller needle-suture combination‚ regardless of filament type‚ to minimize trauma and optimize healing.
Absorbable vs. Non-Absorbable Suture & Size Selection
Absorbable sutures‚ designed for internal tissues‚ often benefit from a slightly larger needle size to ensure secure placement during deeper closures. Their degradation necessitates robust initial fixation.
Non-absorbable sutures‚ used for skin or tissues requiring long-term support‚ can often utilize smaller needle sizes‚ prioritizing cosmetic outcomes and minimizing scarring.
Consider the tissue tension; higher tension demands a stronger suture and potentially a larger needle to prevent cutting through the tissue during placement.
Suture Size Selection by Tissue Type
Tissue characteristics dictate optimal suture size. Delicate tissues‚ like those found in internal organs‚ generally require smaller sutures (e.g.‚ 6-0 to 8-0) to minimize trauma and promote healing.
Denser tissues‚ such as fascia or tendons‚ necessitate larger‚ stronger sutures (e.g.‚ 2-0 to 4-0) to withstand tension. Skin closure often utilizes 3-0 to 5-0‚ balancing strength with cosmetic appearance.
Proper selection prevents tissue strangulation or suture breakage‚ ensuring successful wound approximation.
Skin Closure: Appropriate Suture Sizes
For routine skin closure‚ 3-0‚ 4-0‚ and 5-0 sutures are commonly employed. The choice depends on skin tension and cosmetic considerations. Areas under high tension‚ like joints‚ benefit from 3-0 or 4-0 for increased strength.
Facial skin‚ requiring minimal scarring‚ often utilizes 5-0 or 6-0 for finer results. Smaller sizes reduce the risk of suture marks‚ while larger sizes provide robust wound edge approximation. Careful selection balances functional and aesthetic outcomes.
Subcutaneous Tissue: Recommended Suture Sizes
Closing subcutaneous tissue typically requires 2-0 to 4-0 sutures. This layer demands sufficient strength to minimize dead space and prevent seroma formation‚ but doesn’t necessitate the fine detail of skin closure.
Larger sizes (2-0‚ 3-0) are preferred in areas with significant tension or larger defects‚ providing robust support. 4-0 sutures are suitable for less tense closures. Absorbable sutures are commonly used here‚ eliminating the need for removal.
Fascial Closure: Optimal Suture Sizes
Fascial layers require strong‚ secure closure‚ typically utilizing 0 to 2-0 sutures. The goal is to restore anatomical integrity and prevent herniation‚ demanding high tensile strength. Non-absorbable sutures are often favored for their lasting support.
Heavier fascial repairs may benefit from 0 sutures‚ while 2-0 sutures suffice for thinner fascia or less tension. Precise approximation is vital‚ and careful knot tying is essential to avoid tissue strangulation.
Suture Size Selection by Anatomical Location
Anatomical location significantly influences suture choice. Areas with thin skin and delicate tissues‚ like the face‚ necessitate finer sutures – typically 6-0 or 7-0 – to minimize scarring and maintain cosmetic outcomes. Conversely‚ the scalp‚ with its thicker skin and robust blood supply‚ tolerates larger sutures‚ such as 3-0 or 4-0.
Consideration of tension and cosmetic results are paramount when selecting suture sizes based on anatomical location‚ ensuring optimal wound closure and patient satisfaction.
Facial Suturing: Fine Suture Sizes
Facial skin demands meticulous closure‚ prioritizing aesthetics. Utilizing fine sutures – commonly 6-0 or 7-0 – minimizes scarring and ensures optimal cosmesis. These smaller sizes reduce tissue reaction and tension‚ promoting a more natural healing process. Monofilament sutures are often preferred to reduce inflammation and visibility.
Precise knot tying and gentle handling are essential when employing fine sutures on facial wounds‚ maximizing cosmetic outcomes and patient satisfaction.
Scalp Suturing: Larger Suture Sizes
The scalp‚ with its robust blood supply and thicker tissue‚ necessitates stronger suture materials. Typically‚ 3-0 or 4-0 sutures are employed to achieve secure closure and withstand tension. Due to the scalp’s elasticity and potential for significant movement‚ larger sizes minimize the risk of wound dehiscence.
Cuttting needles are frequently favored for their ability to penetrate dense scalp tissue efficiently‚ ensuring a reliable and durable repair.
Pediatric Suture Size Considerations
Pediatric patients present unique suturing challenges due to their delicate tissues and smaller anatomical structures. Utilizing smaller suture sizes‚ such as 6-0 or 7-0‚ is paramount to minimize scarring and tissue trauma. Fine‚ non-absorbable sutures are often preferred for skin closure‚ promoting optimal cosmetic outcomes.
Careful attention to needle type is also crucial; tapered needles reduce the risk of inadvertent tissue damage during penetration in these vulnerable patients.
Smaller Suture Sizes for Delicate Tissues

When dealing with pediatric patients‚ the selection of appropriately sized sutures is critical for minimizing tissue trauma and optimizing cosmetic results. Sizes ranging from 6-0 to 8-0 are frequently employed due to their reduced tensile strength and finer diameter.
These smaller gauges are less likely to cause excessive tension‚ which can lead to necrosis or wound dehiscence in delicate pediatric tissues. Careful consideration of the tissue type and wound location is essential.
Complications Related to Incorrect Suture Size
Utilizing an inappropriate suture size can significantly compromise wound healing and patient outcomes. Excessive tension from sutures that are too large can restrict blood flow‚ leading to tissue necrosis and delayed healing.
Conversely‚ sutures that are too small may lack sufficient strength‚ resulting in wound eversion or inversion‚ increasing the risk of infection and poor cosmetic appearance. Careful assessment and proper size selection are paramount to avoid these complications.
Tissue Necrosis from Excessive Tension
Applying undue tension with sutures‚ often due to selecting a size too large‚ severely restricts microcirculation to surrounding tissues. This ischemia‚ or lack of blood flow‚ initiates a cascade of cellular damage‚ ultimately leading to tissue necrosis – the death of cells and tissues.
Recognizing early signs like discoloration and compromised wound edges is crucial. Reducing tension through proper suture selection and technique is vital to prevent this serious complication and promote healthy healing.

Wound Eversion/Inversion due to Improper Size
Incorrect suture size selection directly impacts wound edge approximation. A suture that’s too small may lack the tensile strength to adequately bring wound edges together‚ resulting in wound eversion – edges pulled outward. Conversely‚ a suture too large can cause excessive tightening‚ leading to wound inversion – edges rolled inward.
Both scenarios hinder optimal healing and increase the risk of complications. Careful consideration of tissue type and desired cosmetic outcome is paramount for appropriate size choice.